
This AOP is licensed under the BY-SA license. This license allows reusers to distribute, remix, adapt, and build upon the material in any medium or format, so long as attribution is given to the creator. The license allows for commercial use. If you remix, adapt, or build upon the material, you must license the modified material under identical terms.
AOP: 450
Title
Inhibition of AChE and activation of CYP2E1 leading to sensory axonal peripheral neuropathy and mortality
Short name
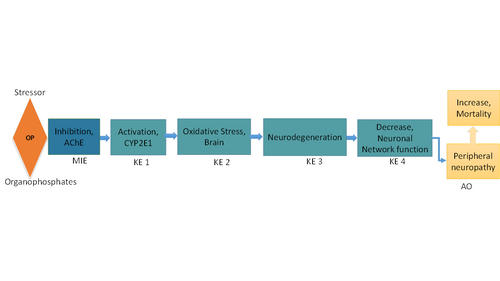
Graphical Representation
Point of Contact
Contributors
- SAROJ AMAR
- Kurt A. Gust
- Allie Always
Coaches
OECD Information Table
| OECD Project # | OECD Status | Reviewer's Reports | Journal-format Article | OECD iLibrary Published Version |
|---|---|---|---|---|
This AOP was last modified on May 26, 2024 20:39
Revision dates for related pages
| Page | Revision Date/Time |
|---|---|
| Acetylcholinesterase (AchE) Inhibition | April 29, 2020 17:21 |
| Activation of Cyp2E1 | June 19, 2021 14:19 |
| Oxidative Stress in Brain | April 04, 2018 14:24 |
| N/A, Neurodegeneration | February 23, 2021 05:07 |
| Decreased, Neuronal network function in adult brain | September 16, 2017 10:15 |
| Increased Mortality | July 08, 2022 07:32 |
| Sensory axonal peripheral neuropathy | January 29, 2019 10:08 |
| AchE Inhibition leads to Activation of Cyp2E1 | May 16, 2022 20:18 |
| Sensory axonal peripheral neuropathy leads to Increased Mortality | May 16, 2022 20:22 |
| Activation of Cyp2E1 leads to Oxidative Stress in Brain | May 16, 2022 20:19 |
| Oxidative Stress in Brain leads to N/A, Neurodegeneration | May 16, 2022 20:20 |
| N/A, Neurodegeneration leads to Decreased, Neuronal network function in adult brain | November 29, 2016 20:24 |
| Decreased, Neuronal network function in adult brain leads to Sensory axonal peripheral neuropathy | May 16, 2022 20:21 |
| Paraoxon | June 24, 2021 18:47 |
| Methyl parathion | June 24, 2021 18:49 |
| Ethyl Parathion | June 24, 2021 18:52 |
| Organophosphates | November 29, 2016 21:20 |
Abstract
Organophosphate compounds (OP) such as paraoxon, ethyl parathion, methyl parathion and others are widely used insecticides. OP compounds are also being developed as warfare nerve agents like soman, sarin and tabun etc. The present adverse outcome pathway (AOP) utilizing the existing key events (KEs) and describes the risk associated with a characteristics OP exposure via acetylcholinesterase (AChE) inhibition as molecular initiating event (MIE), which roots a series of KEs that ultimately manifest the adverse outcomes (AO) of sensory axonal peripheral neuropathy and mortality. The MIE of inhibited AChE triggers the KEs: activation of CYP2E1 (aopwiki.org/events/1508), oxidative stress in brain (aopwiki.org/events/1510), neurodegeneration (aopwiki.org/events/352), decreased neuronal network function in adult brain (aopwiki.org/events/618), sensory axonal peripheral neuropathy (aopwiki.org/events/1583) and increased mortality (aopwiki.org/events/351). The OP insecticides inhibits AChE by inhibition of serine esterases and proteases via phosphorylation (Amitai G et al., 1998, Petroianu GA et al., 2001). Farm workers exposed with commonly used OP showed sharp decrease in blood AChE (MIE) level simultaneously over expression of CYP2E1 (KE1) at mRNA level (Sharma RK et al., 2013). CYP2E1-induced oxidative stress (KE2) by over activation of JNK signaling (Schattenberg JM et al., 2014). Literature further supported that oxidative stress causes neurodegeneration (KE3) by targeting different cellular macromolecules including membrane lipid peroxidation, mitochondrial dysfunction and oxidation of protein and nucleic acid (Gandhi S et al., 2012). Thus neurodegeneration and oxidative stress are inherently related phenomena, since microglia and astrocytes are the main sources of reactive oxygen species in CNS degenerative disorders consequently oxidative stress in brain caused neurodegeneration (Mendonca HR et al., 2020, Wakatsuki S et al., 2015, Mishra V et al., 2015, Kim M et al., 2019). Neurodegeneration leads to impairment of retrograde axonal transport that prohibits the growth factor supply to long-range projection neurons, causing synapse loss, and post-synaptic dendrite retraction that leads to decrease of the neuronal network in adult brain (KE 4) (aopwiki.org/relationships/647, Seeley WW et al., 2009). Palop et al (2006) also advocated that neurodegeneration leads to neural network dysfunction. Consequently, loss of neuronal network function in adult brain leads to an important adverse outcome sensory axonal peripheral neuropathy and symptoms include numbness, lack of coordination, impairment of motor nerve, dizziness, burning sensation etc. (Diantonio et al., 2019, Valek L et al., 2019, Persson AK et al., 2016, Topp KS et al., 2000). Thus this AO represents a disparate group of diseases where epidemiological features indicate the potential for a secondary AO of mortality as final adverse outcome (Taverner T et al., 2019, Martyn CN et al., 1997, Hughes RA et al., 1995). Thus this AOP established the connection between OP chemicals and sensory axonal peripheral neuropathy including mortality to endorse predictive toxicology.
AOP Development Strategy
Context
Strategy
Summary of the AOP
Events:
Molecular Initiating Events (MIE)
Key Events (KE)
Adverse Outcomes (AO)
| Type | Event ID | Title | Short name |
|---|
| MIE | 12 | Acetylcholinesterase (AchE) Inhibition | AchE Inhibition |
| KE | 1391 | Activation of Cyp2E1 | Activation of Cyp2E1 |
| KE | 1510 | Oxidative Stress in Brain | Oxidative Stress in Brain |
| KE | 352 | N/A, Neurodegeneration | N/A, Neurodegeneration |
| KE | 618 | Decreased, Neuronal network function in adult brain | Decreased, Neuronal network function in adult brain |
| AO | 1583 | Sensory axonal peripheral neuropathy | Sensory axonal peripheral neuropathy |
| AO | 351 | Increased Mortality | Increased Mortality |
Relationships Between Two Key Events (Including MIEs and AOs)
| Title | Adjacency | Evidence | Quantitative Understanding |
|---|
| AchE Inhibition leads to Activation of Cyp2E1 | adjacent | Low | Moderate |
| Activation of Cyp2E1 leads to Oxidative Stress in Brain | adjacent | Moderate | Moderate |
| Oxidative Stress in Brain leads to N/A, Neurodegeneration | adjacent | High | High |
| N/A, Neurodegeneration leads to Decreased, Neuronal network function in adult brain | adjacent | High | High |
| Decreased, Neuronal network function in adult brain leads to Sensory axonal peripheral neuropathy | adjacent | Moderate | Low |
| Sensory axonal peripheral neuropathy leads to Increased Mortality | non-adjacent | Low | Low |
Network View
Prototypical Stressors
Life Stage Applicability
| Life stage | Evidence |
|---|---|
| Juvenile | High |
| Adults | Moderate |
Taxonomic Applicability
Sex Applicability
| Sex | Evidence |
|---|---|
| Male | High |
| Female | Moderate |
Overall Assessment of the AOP
Exposure to OP toxicants is the major source of poisoning worldwide, which affecting approximately 3 million populations early, out of which nearly 15% die as a consequence of poisoning (Farizatto KLG et al., 2017; Eddleston et al., 2008). Exposure route of OP pesticide may be drinking contaminated water, breathing vapors of the toxicants, or direct exposure to a person’s skin with the toxicant. Stressor OPs causes inhibition of MIE (AChE) is well documented in literatures. OP pesticides like parathion and chlorpyrifos exercise their toxicity by irreversible inhibition of AChE (Amitai G et al., 1998). Irreversible inhibition of AChE by OPs in birds, insects, fish, and mammals causes neurotoxicity via characteristics cholinergic toxicity (Cao J et al., 2020; Pundir, C. S et al., 2012). AChE hydrolyses acetylcholine into acetic acid and choline, thus terminates the action of the neurotransmitter acetylcholine. This hydrolysis is inhibited by OP pesticides as OP interfere with the breakdown of acetylcholine by binding to the AChE, which resulted in accumulation of acetylcholine in the nerve synapses and triggered interrupted neurotransmission (Thapa S et al., 2017). Thus OP-induced synaptotoxicity is directly associated with MIE (inhibition of AChE). Inhibition of AChE activates the expression of Cytochrome P450 2E1 i.e CYP2E1 (KE1) as reported in farm workers exposed with OP (Sharma RK et al., 2013). A correlation study between inhibited AChE and CYP2E1 induction in mouse brain is reported by Ma JQ et al., 2016. Enzymology study showed that AChE reactivator’s oxime were tested positive for their potential to inhibit CYP2E1 (Spicakova A et al., 2016; Veinlichova A et al., 2009). As previous study reported CYP2E1 a free enzyme with significant pro-oxidant activity is rich source of oxidative stress (Ma JQ, et al., 2016). Thus, in brain the expression of CYP2E1 results in the formation of oxygen radical intermediates and increased oxidative stress (KE2) in the astrocytes of CNS via JNK signaling (Schattenberg JM et al., 2014, Lu Y et al., 2008 Jin, M et al., 2013). Neurodegeneration are characterized by oxidative stress associated disorder with slow and gradual deterioration of structure and function of neurons (Uddin MS et al., 2020). Recent study reported that oxidative stress (KE2) mediated the neurodegeneration (KE3) via mitochondrial dysfunction and excitotoxicity (Uddin MS et al., 2020). Since the main source of oxidative stress in CNS is microglia and astrocytes thus oxidative stresses and neurodegeneration are associated together (Gandhi S et al., 2012). In vitro and in vivo study by Wakatsuki S, et al. (2015) revealed that oxidative stress induced two major pathways of neurodegeneration, neuronal apoptosis and axonal degeneration via phosphorylation dependent ZNFR1 signaling. Previous study suggested that in transgenic mouse model, neurological defects and network dysfunction are associated with neurological diseases (Palop et al., 2006). As per neuropathological inferences, neuroimaging technique, patients suffering from neurodegeneration and the supporting proof from transgenic animal models of neurodegeneration, it’s recommended that neurodegeneration is largely associated with decreased neural network function in adult brain. (aopwiki.org/relationships/647, Palop et al., 2007; Seeley WW et al., 2009). Thus neurodegeneration induced loss of neuronal network function in adult brain. Degeneration of injured axons is characteristics features of peripheral neuropathy as animal models demonstrated that blocking axon degeneration can prevent the development of peripheral neuropathy (DiAntonio. 2019). Axonal degeneration of peripheral sensory neurons is a main clinical index of peripheral sensory neuropathy (Liu H et al., 2017). Axonal degeneration induced peripheral neuropathy via self-destructive pathways and mechanistic study in mammalian model highlighted the three distinct pathways i.e wallerian degeneration, apoptosis-induced axon degeneration and pruning-induced axon degeneration (Geden MJ et al., 2016; DiAntonio et al., 2019). As per existing AOP relationship, impaired axonial transport leads to sensory axonal peripheral neuropathy (aopwiki.org/relationships/1835). The loss of neuronal network function in adult brain (KE4) leads to sensory axonal peripheral neuropathy (AO) with symptoms of numbness, lack of coordination, impairment of motor nerve, dizziness, burning sensation etc. (DiAntonio et al., 2019, Valek L et al., 2019, Persson AK et al., 2016, Topp KS et al., 2000). Axonal neuropathy in childhood causes wasting, weakness and delayed development which impacts nervous system and other systemic manifestation, eventually causes mortality (Yiu EM et al., 2012). Peripheral neuropathy is generally irreversible disease with principle of treatment to prevent the progress of disease and related complications (Azhary H et al., 2010, Hicks CW et al., 2019). Since peripheral neuropathy is desperate group of diseases including several common and rare disease thus possess significant contribution in burden of disease and fatal disability in population (Martyn CN and Hughes RA, 1997). As per latest report Peripheral neuropathy was independently allied with mortality in the U.S. population, conclude that decreased sensation in the foot may be an unpredictable risk factor for death and the incident rate of mortality due to peripheral neuropathy is 34.3 % in the general population (Hicks CW et al., 2021). Consequently this evidence reveals the relation between AO (peripheral neuropathy) with enhanced mortality as terminal AO. Thus this AOP can open the route between MIE and AO that is important to scan the human health assessment specially the individual with potential pesticides exposure risk.
Domain of Applicability
Life Stage Applicability The key molecular target is the AChE enzyme, which appears to be available in all life stages of different species.
|
Life Stage |
Evidence |
|
Child |
High |
|
Adult |
Moderate |
Taxonomic Applicability
|
Term |
Scientific Term |
Evidence |
Links |
|
Homo sapiens |
Homo sapiens |
Moderate |
|
|
Rattus norvegicus |
Rattus norvegicus |
High |
|
|
Mus musculus |
Mus musculus |
High |
Sex Applicability
|
Sex* |
Evidence |
|
Female |
Moderate |
|
Male |
High |
*Study with 44 children for scanning the OP pesticide exposure risk witnessed differences for sex of the child, with male levels higher than female levels (Loewenherz C et al., 1997).
Essentiality of the Key Events
Rationale for essentiality calls:
- MIE: Inhibition, AChE: AChE hydrolyses acetylcholine into acetic acid and choline, thus terminates the action of the neurotransmitter acetylcholine. This hydrolysis is inhibited by OP pesticides as OP interfere with the breakdown of acetylcholine by binding to the AChE, which resulted in accumulation of acetylcholine in the nerve synapses and triggered interrupted neurotransmission (Thapa S et al., 2017). Previous studies with vertebrate and invertebrate validate the dependence of AChE activity to the dose of OP and increasing inhibition of AChE in dose dependent manner with OP as reported in fish, birds, nematodes, rodents and mollusk (https://aopwiki.org/events/12). Inhibition of acetylcholine binding at the serine site results in an accumulation of acetylcholine in synapses with muscarinic and nicotinic receptors which resulting in unregulated excitation at junctions (https://aopwiki.org/events/10).
- Key Event 1: Activation, CYP2E1: CYP2E1 can define as a P450 monooxygenase that activates the substrates by the addition of oxygen and producing an electrophilic metabolite (https://aopwiki.org/aops/220; Smith, et al. 2016). CYP2E1 in its catalytic cycle produce reactive oxygen species and expressed in the different part of human brain including cortex, cerebellum, hippocampus, thalamus and stratum and produce reactive oxygen species in its catalytic cycle. CYP2E1 is linked with oxidative damage of the brain (Jin, M et al., 2013). Activation of CYP2E1 is ultimately associated with the increase production of ROS (aopwiki.org/relationships/1726). Maneb and Paraquate a neurodegenerative pesticide enhanced the expression of CYP2E1 in male wistar rat which causes oxidative stress (Ahmad I et al., 2014). Activity of CYP2E1 is increasing with drugs, anesthetic agents, pesticides and related disorder (García-Suástegui WA et al., 2017) and linked with AChE inhibition as reported in farm worker (Sharma RK et al., 2013). The highest level of CYP2E1 is found in the mitochondria and the endoplasmic reticulum of rat’s brain cells. Expression of CYP2E1 was found in the amygdala and prefrontal cortex in human brain (aopwiki.org/events/1508).
- Key Event 2: Increased, oxidative stress in brain: The association between activation of CYP2E1 and the formation of ROS, which eventually leads to oxidative stress are well documented (https://aopwiki.org/relationships/1726). Study by Haorah et al. (2008) showed that CYP2E1 indeed produces ROS. Oxidative stress leads to neuronal apoptosis and neuronal degeneration by activating ZNRF1 via epidermal growth factor receptor (EGFR)–mediated phosphorylation (Wakatsuki S et al., 2015). ROS is closely associated to neuronal death in several neurological disorders including Parkinson’s and Alzheimer’s disease (Guglielmotto M et al., 2009). Acute injury of the brain including brain trauma and cerebral ischemia (Chen SD et al., 2011) or psychiatric disorders like autism, attention deficit, depression and schizophrenia (Michel TM et al., 2012) are also linked with ROS. ROS may target several different substrates and organelle of the cell like DNA, RNA oxidation, or lipid peroxidation (Gandhi S et al., 2012). ROS induced DNA mutation, DNA-protein crosslinks, DNA strand break and transformed purine and pyridine bases is documented (Gandhi S et al., 2012).
- Key Event 3: Neurodegeneration: Neurodegeneration is the loss of neuron cells in the brain and spinal cord. The loss of neurons can be define in term of ataxia and dementia i.e. functional loss and sensory dysfunction respectively. Each parts of the brain have their own individual function, thus the neurodegeneration is dependent to individual neuronal loss (Uttara, B et al., 2009). Neurodegeneration is a key aspect of a number of diseases called “neurodegenerative diseases". All of these conditions lead to progressive brain damage and neurodegeneration due to decrease of neuronal function. Neurodegeneration and oxidative stress are inherently related phenomena, since microglia and astrocytes are the main sources of reactive oxygen species in CNS degenerative disorders thus oxidative stress in brain caused neurodegeneration (KE5) (Mendonca HR et al., 2020, Wakatsuki S et al., 2015, Mishra V et al., 2015, Kim M et al., 2019). Hence oxidative stress in brain is the requirement for downstream key event Neurodegeneration.
- Key Event 4: Decreased, neuronal function in adult brain: The interaction of neurons is generally consists of a network of several axon terminals connected through synapses to dendrites on other neurons. Once neuron activated, resulted in firing of an electrochemical signal along the axon and it fires only if the total signal received is above firing threshold (aopwiki.org/events/618). In the brain, neurons create a network where the activity of one cell directly influences many others. Neurotransmitters are released at synaptic transmission by presynaptic neuron which further activate the receptors of the postsynaptic neuron (aopwiki.org/events/618). Synaptic transmission relies on: the availability of the neurotransmitter and the binding of the postsynaptic receptor by the neurotransmitter. Once nerve impulse attains at the synapse, the neurotransmitters releases, which influence postsynaptic neuron. The postsynaptic neurons obtain inputs from both excitatory and inhibitory neurons. The excitatory and inhibitory stimuluses all together causing inhibition or "firing" and the inhibition of AChE resulted in decrease of neuronal function (Kolb and Whishaw, 2003). Previous study confirm the inhibition of AChE by OP pesticides paraoxon and chlorpyrifos and study further reported that environmental exposure of chlorpyrifos may leads to sensory peripheral neuropathy in human (Amitai G et al., 1998).
- Adverse Outcome: Sensory axonal peripheral neuropathy: The most common neurodegenerative syndrome affecting millions of patients worldwide is Peripheral neuropathy. Peripheral neuropathy affect the motor and autonomic systems are due to axonal loss, consequently loss of neuronal function in adult brain leads to an important adverse outcome Sensory axonal peripheral neuropathy (DiAntonio et al., 2019, Valek L et al., 2019, Persson AK et al., 2016, Topp KS et al., 2000). Depending on the exposure level, some of the acute effects of OPs may leads to excessive secretions, cardiorespiratory depression and life threatening seizures. A number of long-term neurological and psychiatric consequences have been observed in survivors with acute OP exposure (Naughton SX et al., 2018). The symptoms may include sustained attention, motor impairments, psychotic episodes, depressed mood and cognitive flexibility (Steenland K et al., 1994; Pereira EF et al., 2014; Rosenstock et al., 1991; Dassanayake et al., 2007). Reversibility of neuropathy upon discontinuation of treatment is also reported (Brown, T et al., 1991). Peripheral neuropathies mostly affect sensory neurons in a length-dependent manner and therefore characterized by a stocking-and-glove distribution of the symptoms and numbness and paresthesia like sensory symptoms (Forsyth, P.a., et al. 1997, aopwiki.org/events/1583).
- Adverse Outcome Terminal: Increased, Mortality Increased mortality refers to an increase in the number of individuals dying in an experimental replicate group or in a population over a specific period of time (aopwiki.org/events/351). It has been estimated that there are 258,234 (plausible range 233,997 to 325,907) deaths from pesticide self-poisoning worldwide yearly, accounting for 30% (range 27% to 37%) of suicides globally (Gunnell D et al., 2007). Peripheral neuropathies are a disparate group of diseases their contribution to the burden of disease and disability is plausible, however there are limited epidemiological evidence that quantitatively connecting the previous AO to mortality rates with regard to the final adverse outcome (Taverner T et al., 2019, Martyn CN et al., 1997, Hughes RA et al., 1995). As per latest report Peripheral neuropathy was independently allied with mortality in the U.S. population, concluded that decreased sensation in the foot may be an unpredictable risk factor for death thus the incident rate of mortality due to peripheral neuropathy is 34.3 % in the general population (Hicks CW et al., 2021). Study in vertebrate and invertebrate showed that 70 to 80 % inhibition of AChE in brain leads to significant increase in mortality via accumulation of ACh (Russom CL et al., 2014).
Evidence Assessment
"'Biological Plausibility"'
OP induced inhibition of AChE leads to accumulation of acetylcholine (ACh) at the cholinergic synaptic clefts, resulting in to long-term activation of the nicotinic and muscarinic ACh receptors (AChR) and overstimulation of cholinergic neurons with hyper excitation and seizures (Faria, M et al., 2015; Peña Llopis, S. & Pena, 2005). OP induced seizures can grow to status epilepticus causing severe damage of brain (Weissman, B. A. & Raveh, L et al., 2008). Inhibition of AChE is associated with wide range of adverse effect including fatality, hence it’s dependent to concentration and half-life of OP dose. Major adverse effects with accumulation of ACh in peripheral system includes glandular secretions, skeletal muscle twitching, smooth muscle contractions and flaccid paralysis, simultaneously centrally mediated impacts associated with learning, memory and behavioral impairments (https://www.epa.gov/sites/production/files/2015-07/documents/cholin.pdf). Oxidative stress is the key mechanisms involved in OP induced neurotoxicity, which can caused by over-production of reactive oxygen species (ROS) in the electron transport system and metabolism of agents by cytochrome P450 (Farkhondeh T et al., 2020). Thus the oxidative stress is inducer of neuronal apoptosis and axonal degeneration. Since it activate the ZNRF1 by inducing epidermal growth factor receptor (EGFR)–mediated phosphorylation at the 103rd tyrosine residue thus the up-regulation of ZNRF1 activity by oxidative stress leads to neuronal apoptosis and Wallerian degeneration (Wakatsuki S et al., 2015). As per neuropathological outcomes and neuroimaging of patients suffering from neurodegeneration as well as complementary evidence from transgenic animal models of neurodegeneration, it has been recommended that neurodegeneration is related to neural network dysfunction (aopwiki.org/relationships/368; Palop et al., 2007b; Seeley WW et al., 2009). Neurodegeneration leads to impairment of retrograde axonal transport that prohibits the growth factor supply to long-range projection neurons, causing synapse loss and post-synaptic dendrite retraction that leads to decreases of the neuronal network (Seeley WW et al., 2009) (https://aopwiki.org/relationships/647). Defective axonal transport are the major cause for peripheral neuropathies as the length-dependent and distal neurologic deficits observed in patients with axonal loss, which are often linked to axonal transport defects ( https://aopwiki.org/relationships/1835 ; Rowinsky, E.K et al., 1995). Mutations linked to axonal transport are known cause of Charcot-Marie-Tooth disease (a peripheral neuropathy) (Zhao, C et al., 2001). Thus the function of axon survival and axon degeneration proteins play an important role in the mechanistic insight. Usually, the clinical presentation reflects an axonal peripheral neuropathy with glove-and-stocking distribution sensory loss, collective with the features indicative of nerve hyper excitability includes paresthesia, dysesthesia, and pain. Symptoms like proprioceptive and motor effects may be prolonged, severe disabling and adversely affect activities of daily living and quality of life (Bhutani M et al., 2010).
"'Concordance of dose-response relationships:"'
Impairments in axonal transport could be detected even at concentrations that did not inhibit AChE activity and they were not blocked by cholinergic receptor antagonists (Naughton SX et al., 2018). Both neuronal culture and animal studies have reported that OP- induced axonal transport deficits as a potential non-cholinesterase mechanism for the long-term deleterious neurological effects (Naughton SX et al., 2021). Physostigmine was establish to strongly inhibit the purified eel AChE with an IC50 of 0.02 μM but not impaired axonal transport (Naughton SX et al., 2021).
"'Temporal concordance among the key events and adverse effect:"'
Sufficient literature evident that around 25 -32% of the US veterans deployed in Persian Gulf War was reported with chronic health symptoms like headache, respiratory problems, musculoskeletal pain and a number of neurological and neuropsychiatric illness including cognitive defects (Naughton SX et al., 2018; Sullivan et al., 2018), inline with exposure of OP based inhibitors of AChE (Winkenwerder, 2003). Depending to exposure level, the effect of OP exposure may include cardiorespiratory depression, life threatening seizures and long term neurological and psychiatric consequences in survival including motor impairment (Naughton SX et al., 2018; Pereira et al., 2014). As per previous report the animal models have been largely appreciated to reveal the effects of anti- AChE abuses and their connection to brain damage in humans. Harrison et al., (2004) establish that OP (Paraoxon) caused seizures in guinea pigs similar to those caused by the nerve gas soman in humans. Similarly, the anti-AChE strength of Paraoxon was similar in macaques and humans (Worek et al., 2011). Moreover, Rosenberg et al., (2017) showed that anti- AChE exposed macaques presented severe signs of toxicity such as fasciculations, miosis, salivation and convulsions including fatality in less than seven hours of application.
"'Consistency:"'
The cholinergic phase typically last within 48 hrs including medical emergency in intensive care unit (Senanayake N et al., 1987). OP induced inhibition of AChE caused accumulation of ACh at muscarinic sites and resulted in secretions, bronchoconstriction, blur vision and bradycardia. Accumulation of ACh at nicotinic sites triggered flaccid paralysis, insomnia, confusion, drowsiness convulsions, coma, and respiratory depression (PMCID: PMC6357250, EJIFCC. 1999). Peripheral neuropathy is the most common neurodegenerative disorder, caused by damaging to peripheral nerves and is an important cause of neuropathic pain including hyperalgesia, allodynia, and dysesthesias (DiAntonio et AL et al., 2019). Acute exposure of organophosphate induced delayed neuropathy is well reported which is characterized by distal degeneration of axons of CNS and PNS. Non excitability of the nerve with electromyographical signs of denervation has been noticed with progression of disease and the experimental date with human shows recovery in the young (Lotti M., 2005). Transcutaneous intoxication with OP showed the nicotinic effect in young children (Pavlovic M., 2015). A study by Yonggang Li et al (2012) reported that Adult male Sprague Dawley rats treated with acute exposure of OP (diisopropylfluorophosphate) showed that almost all animals developed severe seizures and died within 30 minutes but with delayed neuronal injury model, animal survived and delayed neuronal injury was observed till 4-72 hrs (Li Y et al., 2011). Furthermore the role of oxidative stress in neuronal injury and oxidative stress-mediated protein damage in the brains of diisopropylfluorophosphate -intoxicated rats is also documented (Li Y et al., 2012).
"'Uncertainties, inconsistencies, and data gaps:"'
Cholinergic hyper stimulation which affect nervous system via AChE inhibition is very common mode of action of OP (Pope CN et al., 1999), simultaneously the mouse lacking AChE also showed hyper sensitive of OP via non AChE mechanisms of action (Duysen EG et al., 2001). Unfortunately, the very limited evidence are available for the measurement of AChE inhibition in peripheral neural tissues or neuro-effector junctions. Reductions in neural AChE activity may not always associated with obvious clinical signs because critical functions of those specific neurons may not be sufficiently evaluated to identify associated changes or tolerance developed. The time at which potential functional effects are evaluated may also contribute to an apparent lack of concordance between functional effects and cholinesterase inhibition. Thus it is difficult to determine, with accuracy or consistently, the degree of cholinesterase inhibition that will cause specific physiological or behavioral changes (https://www.epa.gov/sites/production/files/2015-07/documents/cholin.pdf). The existing evidence mostly focused on the whole brain AChE activity, but not usually regional brain measurements, or time-course data, mainly with acute exposures. Thus this is a major limitation, and also the distribution of cholinergic pathways, their concentration and molecular form of AChE in different brain regions is not uniform. Thus, whole brain measurements of AChE inhibition may tell little or no change in activity, while masking significant changes in specific brain regions linked with particular cholinergically-mediated functions can tell more (https://www.epa.gov/sites/production/files/2015-07/documents/cholin.pdf).
Known Modulating Factors
Quantitative Understanding
OP is commonly used as insecticides because it inhibits the AChE of insects (Tomlin C et al., 1994) and the same characteristic mode of cholinergic toxicity has been reported in human (Taylor P et al., 1996). Previous study showed that OP is more effective inhibitor of AChE than neuropathy target esterage (NTE) which causing delayed polyneuropathy at higher dose (Lotti M et al., 1992; Moretto A et al., 1998), simultaneously patients with low level repeated exposure of OP developed sensory neuropathy (Kaplan JG et al., 1993; Moretto A et al., 1998). Inhibition of AChE (MIE) is considered a vital event in the mechanism of cholinergic toxicity, the AChE-inhibiting OP causes a broad range of adverse effects including sensory, cognitive, and psychological effects (Reigart, R. and Roberts, 1999). Decreasing AChE level and increasing CYP2E1 (KE1) is reported in farm worker (Sharma RK et al., 2013). CYP2E1-induced oxidative stress (KE2) (Schattenberg JM et al., 2014) causes neurodegeneration (KE3) (Gandhi S et al., 2012) that leads to dysfunction of neuronal function (Palop et al., 2006). Subsequently, the loss of neuronal network function (KE4) leads to an adverse outcome of sensory axonal peripheral neuropathy (AO) and the symptoms may include lack of coordination, impairment of motor nerve, dizziness, burning sensation, numbness etc. (DiAntonio et al., 2019). This desperate group of diseases due to peripheral neuropathy causes fatal disability and mortality (AO) in population (Martyn CN and Hughes RA, 1997). As per latest report Peripheral neuropathy was self-sufficiently allied with mortality in the U.S. population, concluded that decreased sensation in the foot may be an unpredictable risk factor for death and the rate of mortality associated with peripheral neuropathy is 34.3 % in the general population (Hicks CW et al., 2021). Thus clinical symptoms with behavioral or physiological effects is the most direct evidence of the potential adverse consequences of human exposure to anticholinesterase pesticides like OP (https://www.epa.gov/sites/production/files/2015-07/documents/cholin.pdf).
Considerations for Potential Applications of the AOP (optional)
The potential application of this AOP includes risk assessment in predictive modeling of OP pesticide toxicity via AChE dependent pathways. Thus this AOP is an attempt to create the mechanism of organophosphorus (OP) pesticides induced sensory peripheral neuropathy and mortality as an adverse outcome. Supplementary evidence may help this AOP to fully elucidate the mechanistic approach and the neurotoxic potential of OP pesticide.
References
Ahmad I, Shukla S, Singh D, Chauhan AK, Kumar V, Singh BK, Patel DK, Pandey HP, Singh C. CYP2E1-mediated oxidative stress regulates HO-1 and GST expression in maneb- and paraquat-treated rat polymorphonuclear leukocytes. Mol Cell Biochem. 2014 Aug;393 (1-2) :209-22. doi: 10.1007/s11010-014-2062-y.
Amitai G, Moorad D, Adani R, Doctor BP. Inhibition of acetylcholinesterase and butyrylcholinesterase by chlorpyrifos-oxon. Biochem Pharmacol. 1998; 56(3):293-299. Doi: 10.1016/s0006-2952(98)00035-5
Azhary H, Farooq MU, Bhanushali M, Majid A, Kassab MY. Peripheral neuropathy: differential diagnosis and management. Am Fam Physician. 2010 Apr 1; 81(7):887-92. PMID: 20353146.
Bhutani, Ma & Colucci, P & Laird-F, Heather & Conley, Barbara. (2011). Management of paclitaxel-induced neurotoxicity. Oncology Reviews. 4. 107-115. 10.1007/s12156-010-0048-x.
Brown, T., et al., A phase I trial of taxol given by a 6-hour intravenous infusion. Journal of Clinical Oncology, 1991. 9(7): p. 1261-1267.
Cao J, Wang M, Yu H, She Y, Cao Z, Ye J, Abd El-Aty AM, Hacımüftüoğlu A, Wang J, Lao S. An Overview on the Mechanisms and Applications of Enzyme Inhibition-Based Methods for Determination of Organophosphate and Carbamate Pesticides. J Agric Food Chem. 2020 Jul 15; 68(28):7298-7315. doi: 10.1021/acs.jafc.0c01962. Epub 2020 Jul 2. PMID: 32551623.
Chen SD, Yang DI, Lin TK, Shaw FZ, Liou CW, Chuang YC. Roles of oxidative stress, apoptosis, PGC-1α and mitochondrial biogenesis in cerebral ischemia. Int J Mol Sci. 2011; 12(10):7199-215. doi: 10.3390/ijms12107199. Epub 2011 Oct 21. PMID: 22072942; PMCID: PMC3211033.
Dassanayake T, Weerasinghe V, Dangahadeniya U, Kularatne K, Dawson A, Karalliedde L, Senanayake N. (2007) Cognitive processing of visual stimuli in patients with organophosphate insecticide poisoning. Neurology 68:2027–30. doi: 10.1212/01.wnl.0000264423.12123.f0
Deshpande LS, Phillips K, Huang B, DeLorenzo RJ (September 2014). "Chronic behavioral and cognitive deficits in a rat survival model of paraoxon toxicity". Neurotoxicology. 44: 352–7.
DiAntonio A. Axon degeneration: mechanistic insights lead to therapeutic opportunities for the prevention and treatment of peripheral neuropathy. Pain. 2019; 160 Suppl 1:S17-S22. doi:10.1097/j.pain.0000000000001528
Duysen EG, Li B, Xie W, Schopfer LM, Anderson RS, et al. Evidence for Nonacetylcholinesterase Targets of Organophosphorus Nerve Agent: Supersensitivity of Acetylcholinesterase Knockout Mouse to VX Lethality. J Pharmacol Exp Ther. 2001; 299:528–535.
Eddleston M, Gunnell D, Karunaratne A, de Silva D, Sheriff MH, Buckley NA. Epidemiology of intentional self-poisoning in rural Sri Lanka. The British Journal of Psychiatry. 2005;187:583–584.
Faria, M. et al. Zebrafish Models for Human Acute Organophosphorus Poisoning. Sci. Rep. 5, 15591; doi: 10.1038/srep15591 (2015)
Farizatto KLG, Bahr BA. Paraoxon: An Anticholinesterase That Triggers an Excitotoxic Cascade of Oxidative Stress, Adhesion Responses, and Synaptic Compromise. Eur Sci J. 2017; 13:29-37. doi:10.19044/esj.2017.c1p4
Farkhondeh, T., Mehrpour, O., Forouzanfar, F. et al. Oxidative stress and mitochondrial dysfunction in organophosphate pesticide-induced neurotoxicity and its amelioration: a review. Environ Sci Pollut Res 27, 24799–24814 (2020). https://doi.org/10.1007/s11356-020-09045-z.
Forsyth, P.a., et al., Prospective study of paclitaxel-induced peripheral neuropathy with quantitative sensory testing. Journal of Neuro-Oncology, 1997. 35(1): p. 47-53.
Gandhi S, Abramov AY. Mechanism of Oxidative Stress in Neurodegeneration. Oxid Med Cell Longev. 2012; 2012:428010.
Garcia S , Abu-Qare A, Meeker-O'Connell W, Borton A & Abou-Donia M (2003) Methyl Parathion: A Review of Health Effects, Journal of Toxicology and Environmental Health Part B: Critical Reviews, 6:2, 185-210, DOI: 10.1080/10937400306471.
García-Suástegui WA, Ramos-Chávez LA, Rubio-Osornio M, Calvillo-Velasco M, Atzin-Méndez JA, Guevara J, et al. The Role of CYP2E1 in the Drug Metabolism or Bioactivation in the Brain. Oxid Med Cell Longev. 2017; 2017:4680732-.
Garciá-Suástegui, W. A. et al. The Role of CYP2E1 in the Drug Metabolism or Bioactivation in the Brain. Oxidative Medicine and Cellular Longevity (2017).
Geden MJ, Deshmukh M. Axon degeneration: context defines distinct pathways. Curr Opin Neurobiol. 2016; 39:108-115. doi:10.1016/j.conb.2016.05.002
Guglielmotto M, Tamagno E, Danni O. Oxidative Stress and Hypoxia Contribute to Alzheimer's disease Pathogenesis: Two Sides of the Same Coin. TheScientific World JOURNAL. 2009; 9:195783.
Gunnell D, Eddleston M, Phillips MR, Konradsen F. The global distribution of fatal pesticide self-poisoning: systematic review. BMC Public Health. 2007; 7:357. Published 2007 Dec 21. doi:10.1186/1471-2458-7-357.
Haorah, J. et al. Mechanism of alcohol-induced oxidative stress and neuronal injury. Free Radic. Biol. Med. 45, 1542–1550 (2008).
Harrison PK, Sheridan RD, Green AC, Scott IR, Tattersall JE. A guinea pig hippocampal slice model of organophosphate-induced seizure activity. Journal of Pharmacology and Experimental Therapeutics. 2004; 310:678–686.
Hicks CW, Selvin E. Epidemiology of Peripheral Neuropathy and Lower Extremity Disease in Diabetes. Curr Diab Rep. 2019 Aug 27; 19(10):86. doi: 10.1007/s11892-019-1212-8. PMID: 31456118; PMCID: PMC6755905.
Hicks CW, Wang D, Matsushita K, and Windham BG, Selvin E. Peripheral Neuropathy and All-Cause and Cardiovascular Mortality in U.S. Adults: A Prospective Cohort Study. Ann Intern Med. 2021 Feb; 174(2):167-174. doi: 10.7326/M20-1340. Epub 2020 Dec 8. PMID: 33284680;
Hill RH Jr, Alley CC, Ashley DL, Cline RE, Head SL, Needham LL, et al. Laboratory investigation of a poisoning epidemic in Sierra Leone. J Anal Toxicol 1990; 14(4):213-216.
Hughes RA. Epidemiology of peripheral neuropathy. Curr Opin Neurol. 1995;8(5):335-338. doi:10.1097/00019052-199510000-00001.
Jaga K, Dharmani C. Methyl parathion: an organophosphate insecticide not quite forgotten. Rev Environ Health 2006; 21(1):57-67.
Jin, M., Ande, A., Kumar, A. et al. Regulation of cytochrome P450 2e1 expression by ethanol: role of oxidative stress-mediated pkc/jnk/sp1 pathway. Cell Death Dis 4, e554 (2013). https://doi.org/10.1038/cddis.2013.78
Johnson FO, Chambers JE, Nail CA, Givaruangsawat S, Carr RL. Developmental chlorpyrifos and methyl parathion exposure alters radial-arm maze performance in juvenile and adult rats. Toxicol Sci. 2009; 109(1):132-142. doi:10.1093/toxsci/kfp053.
Kaplan JG, Kessler J, Rosenberg N, et al. Sensory neuropathy associated with Dursban (chlorpyrifos) exposure. Neurology 1993; 43:2193–6
Kim M, Kim H, Kim D, et al. Heme Oxygenase 1 in Schwann Cells Regulates Peripheral Nerve Degeneration Against Oxidative Stress. ASN Neuro. 2019; 11:1759091419838949. doi:10.1177/1759091419838949
Kolb, Bryan; Whishaw, Ian Q., Fundamentals of Human Neuropsychology (5th ed.). 2003, Worth. pp. 102–104. ISBN 978-0-7167-5300-1.
Laxmikant S. Deshpande, Dawn S. Carter, Kristin F. Phillips, Robert E. Blair, Robert J. DeLorenzo, Development of status epilepticus, sustained calcium elevations and neuronal injury in a rat survival model of lethal paraoxon intoxication, NeuroToxicology (2014), Volume 44,2014,Pages 17-26
Li Y, Lein PJ, Liu C, Bruun DA, Tewolde T, Ford G, Ford BD. Spatiotemporal pattern of neuronal injury induced by DFP in rats: A model for delayed neuronal cell death following acute OP intoxication. Toxicology and Applied Pharmacology. 2011; 253:261–269.
Li Y, Lien PJ, Liu C, et al. Neuregulin-1 is neuroprotective in a rat model of organophosphate-induced delayed neuronal injury. Toxicol Appl Pharmacol. 2012; 262(2):194-204. doi:10.1016/j.taap.2012.05.001
Liu H, Wu C. Charcot Marie Tooth 2B Peripheral Sensory Neuropathy: How Rab7 Mutations Impact NGF Signaling? Int J Mol Sci. 2017 Feb 4; 18(2):324. doi: 10.3390/ijms18020324. PMID: 28165391; PMCID: PMC5343860.
Loewenherz C et al. Biological monitoring of organophosphorus pesticide exposure among children of agricultural workers in Central Washington State. Environ Health Persp 1997, 105:1344
Lores EM, Bradway DE, Moseman RF. Organophosphorus pesticide poisonings in humans: determination of residues and metabolites in tissues and urine. Arch Environ Health 1978; 33(5):270-276.
Lotti M, Moretto A. Organophosphate-induced delayed polyneuropathy. Toxicol Rev. 2005; 24(1):37-49. doi: 10.2165/00139709-200524010-00003. PMID: 16042503.
Lotti M. The pathogenesis of organophosphate delayed polyneuropathy. Crit Rev Toxicol 1992; 21:465–87.
Lu Y, Cederbaum AI. CYP2E1 and oxidative liver injury by alcohol. Free Radic Biol Med. 2008; 44(5):723-38.
Ma JQ, Luo RZ, Jiang HX, Liu CM. Quercitrin offers protection against brain injury in mice by inhibiting oxidative stress and inflammation. Food Funct. 2016 Jan; 7(1):549-56. doi: 10.1039/c5fo00913h. PMID: 26510118.
Martyn CN, Hughes RA. Epidemiology of peripheral neuropathy. J Neurol Neurosurg Psychiatry. 1997; 62(4):310-318. doi:10.1136/jnnp.62.4.310
Mendonca HR, Carpi-Santos R, da Costa Calaza K, Blanco Martinez AM. Neuroinflammation and oxidative stress act in concert to promote neurodegeneration in the diabetic retina and optic nerve: galectin-3 participation. Neural Regen Res. 2020; 15(4):625-635. doi:10.4103/1673-5374.266910
Michel TM, Pülschen D, Thome J. The role of oxidative stress in depressive disorders. Curr Pharm Des. 2012; 18(36):5890-9. doi: 10.2174/138161212803523554. PMID: 22681168.
Mishra V, Shuai B, Kodali M, et al. Resveratrol Treatment after Status Epilepticus Restrains Neurodegeneration and Abnormal Neurogenesis with Suppression of Oxidative Stress and Inflammation. Sci Rep. 2015; 5:17807. Published 2015 Dec 7. doi:10.1038/srep17807
Moretto A, Lotti M. Poisoning by organophosphorus insecticides and sensory neuropathy. J Neurol Neurosurg Psychiatry. 1998 Apr; 64(4):463-8. doi: 10.1136/jnnp.64.4.463. PMID: 9576536; PMCID: PMC2170059.
Naughton SX, Beck WD, Wei Z, Wu G, Baas PW, Terry AV Jr. The Carbamate, Physostigmine does not Impair Axonal Transport in Rat Cortical Neurons. Neurosci Insights. 2021; 16:26331055211020289. Published 2021 May 24. Doi: 10.1177/26331055211020289
Naughton SX, Terry AV Jr. Neurotoxicity in acute and repeated organophosphate exposure. Toxicology. 2018; 408:101-112. doi:10.1016/j.tox.2018.08.011
Organophosphorus Insecticide Poisoning. EJIFCC. 1999; 11(2):30-35. Published 1999 Jul 7.
Palop J.J, J. Chin, E.D. Roberson, J. Wang, M.T. Thwin, N. Bien-Ly, J. Yoo, K.O. Ho, G.Q. Yu, A. Kreitzer, et al., Aberrant excitatory neuronal activity and compensatory remodeling of inhibitory hippocampal circuits in mouse models of Alzheimer's disease. Neuron, 2007, 55: 697–711.
Palop J.J., J. Chin, L. Mucke, A network dysfunction perspective on neurodegenerative diseases. Nature, 2006, 443: 768–773.
Pavlovic M, Neubauer D, Al-Tawari AA. Delayed Effects of Transcutaneous Organophosphate Poisoning in Four Children. Child Neurol Open. 2015 Nov 27; 2(4):2329048X15618970. doi: 10.1177/2329048X15618970. PMID: 28503600; PMCID: PMC5417017
Peña Llopis, S. & Pena, L. Antioxidants as Potentially Safe Antidotes for Organophosphorus Poisoning. Current enzyme inhibition 1, 147–156 (2005).
Pereira EF, Aracava Y, DeTolla LJ Jr, Beecham EJ, Basinger GW Jr, Wakayama EJ, Albuquerque EX. (2014). Animal models that best reproduce the clinical manifestations of human intoxication with organophosphorus compounds. J Pharmacol Exp Ther. 350(2):313–321. doi: 10.1124/jpet.114.214932
Persson AK, Hoeijmakers JGJ, Estacion M, Black JA, Waxman SG. Sodium Channels, Mitochondria, and Axonal Degeneration in Peripheral Neuropathy. Trends Mol Med. 2016 May; 22(5):377-390. doi: 10.1016/j.molmed.2016.03.008. Epub 2016 Apr 13. PMID: 27085813.
Petroianu GA, Hasan MY, Arafat K, Nurulain SM, Schmitt A. Weak inhibitors protect cholinesterases from strong inhibitors (paraoxon): in vitro effect of tiapride. J Appl Toxicol. 2005; 25(6):562-567. doi: 10.1002/jat.1097
Pope CN, Brimijoin S. Cholinesterases and the fine line between poison and remedy. Biochem Pharmacol. 2018; 153:205-216. doi:10.1016/j.bcp.2018.01.044
Pundir, C. S.; Chauhan, N. Acetylcholinesterase inhibition-based biosensors for pesticide determination: a review. Anal. Biochem. 2012, 429 (1), 19−31.
Reigart, R. and Roberts, J. Recognition and Management of Pesticide Poisonings, 5th Edition. US EPA (US Environmental Protection Agency, Washington, DC EPA 735-R98-003. pp. 34 54
Rosenberg YJ, Mao L, Jiang X, Lees J, Zhang L, Radic Z, Taylor P. Post-exposure treatment with the oxime RS194B rapidly reverses early and advanced symptoms in macaques exposed to sarin vapor. Chemico-Biological Interactions. 2017; 274:50–57
Rosenstock L, Keifer M, Daniell WE, McConnell R, Claypoole K. (1991) Chronic central nervous system effects of acute organophosphate pesticide intoxication. The Pesticide Health Effects Study Group. Lancet. July 27;338(8761):223–7
Rowinsky , E.K. and R.C. Donehower Paclitaxel (Taxol). New England Journal of Medicine, 1995. 332(15): p. 1004-1014.
Russom CL, LaLone CA, Villeneuve DL, Ankley GT. Development of an adverse outcome pathway for acetylcholinesterase inhibition leading to acute mortality. Environ Toxicol Chem. 2014 Oct; 33(10):2157-69. doi: 10.1002/etc.2662. Epub 2014 Aug 25. PMID: 24922588.
Schattenberg JM, Czaja MJ. Regulation of the effects of CYP2E1-induced oxidative stress by JNK signaling. Redox Biol. 2014; 3:7-15.
Seeley WW, Crawford RK, Zhou J, Miller BL, Greicius MD. Neurodegenerative diseases target large-scale human brain networks. Neuron. 2009;62(1):42-52. doi:10.1016/j.neuron.2009.03.024.
Senanayake N, Karalliedde L: Neurotoxic effects of organophosphorus insecticides: An intermediate syndrome. N Engl J Med 1987; 316:761- 763.
Sharma RK, Upadhyay G, Siddiqi NJ, Sharma B. Pesticides-induced biochemical alterations in occupational North Indian suburban population. Hum Exp Toxicol. 2013 Nov; 32(11):1213-27. doi: 10.1177/0960327112474835. Epub 2013 Feb 19. PMID: 23424210.
Smith, M.T., Guyton, K.Z., Gibbons, C.F., Fritz, J.M., Portier, C.J., Rusyn, I., DeMarini, D.M., Caldwell, J.C., Kavlock, R.J., Lambert, P., Hecht, S.S., Bucher, J.R., Stewart, B.W., Baan, R., Cogliano, V.J., Straif, K. Key Characteristics of Carcinogens as a Basis for Organizing Data on Mechanisms of Carcinogenesis. Environ. Health Perspect. 2016 06; 124(6):713-21
Spicakova A, Anzenbacher P, Liskova B, Kuca K, Fusek J, Anzenbacherova E. Evaluation of possible inhibition of human liver drug metabolizing cytochromes P450 by two new acetylcholinesterase oxime-type reactivators. Food Chem Toxicol. 2016 Feb; 88:100-4. doi: 10.1016/j.fct.2015.11.024. Epub 2015 Dec 31. PMID: 26747974.
Steenland K, Jenkins B, Ames RG, O’Malley M, Chrislip D, Russo J. (1994) Chronic neurological sequelae to organophosphate pesticide poisoning. Am.J.Public Health 84; 731–6.
Straus, D. L., Schlenk, D., and Chambers, J. E. 2000. Hepatic microsomal desulfuration and dearylation of chlorpyrifos and parathion in fingerling channel catfish: Lack of effect from Aroclor 1254. Aquat. Toxicol. 50:141–149.
Sullivan K, Krengel M, Bradford W, Stone C, Thompson TA, Heeren T and White RF. (2018) Neuropsychological functioning in military pesticide applicators from the Gulf War: Effects on information processing speed, attention and visual memory. Neurotoxicol Teratol. Jan-Feb; 65:1–13. doi: 10.1016/j.ntt.2017.11.002.
Taverner T, Crowe FL, Thomas GN, et al. Circulating Folate Concentrations and Risk of Peripheral Neuropathy and Mortality: A Retrospective Cohort Study in the U.K. Nutrients. 2019; 11(10):2443. Published 2019 Oct 14. doi: 10.3390/nu11102443
Taylor P. Anticholinesterase agents. In: Hardman JG, Limbird LE, eds. Goodman and Gilman’s the pharmacological basis of therapeutics, 9th ed. New York: McGraw Hill, 1996:161–76
Thapa S, Min Lv and Xu H, “Acetylcholinesterase: A Primary Target for Drugs and Insecticides”, Mini-Reviews in Medicinal Chemistry 2017; 17(17). https://doi.org/10.2174/1389557517666170120153930
Tomlin C, ed. The pesticide manual. A world compendium, 10th ed. Bath: British Crop Protection Council, 1994.
Topp KS, Tanner KD, Levine JD. Damage to the cytoskeleton of large diameter sensory neurons and myelinated axons in vincristine-induced painful peripheral neuropathy in the rat. J Comp Neurol. 2000; 424(4):563-576.
U.S. Environmental Protection Agency (U.S. EPA). R.E.D. Facts. Ethyl parathion. September 2000. EPA-738-FOO-009. Available at URL: https://www.epa.gov/oppsrrd1/REDs/factsheets/0155fct.pdfpdf iconexternal icon.1/24/13.
Uddin MS, Al Mamun A, Kabir MT, Ahmad J, Jeandet P, Sarwar MS, Ashraf GM, Aleya L. Neuroprotective role of polyphenols against oxidative stress-mediated neurodegeneration. Eur J Pharmacol. 2020 Nov 5; 886:173412. doi: 10.1016/j.ejphar.2020.173412. Epub 2020 Aug 13. PMID: 32771668.
United States, Environmental Protection Agency. Office of Pesticide Programs. (2000). The Use of Data on Cholinesterase Inhibition for Risk Assessments of Organophosphorous and Carbamate Pesticides. https://www.epa.gov/sites/production/files/2015 07/documents/cholin.pdf accessed Nov. 2018.
Uttara, B., Singh, A. V, Zamboni, P. & Mahajan, R. T. Oxidative stress and neurodegenerative diseases: a review of upstream and downstream antioxidant therapeutic options. Curr. Neuropharmacol. 7, 65–74 (2009).
Valek L, Auburger G, Tegeder I. Sensory neuropathy and nociception in rodent models of Parkinson's disease. Dis Model Mech. 2019; 12(6):dmm039396. Published 2019 Jun 27. doi:10.1242/dmm.039396.
Veinlichova A, Jancova P, Siller M, Anzenbacher P, Kuca K, Jun D, Fusek J, Anzenbacherova E. Effect of acetylcholinesterase oxime-type reactivators K-48 and HI-6 on human liver microsomal cytochromes P450 in vitro. Chem Biol Interact. 2009 Aug 14; 180(3):449-53. doi: 10.1016/j.cbi.2009.03.016. Epub 2009 Mar 31. PMID: 19539805.
Viñuela A, Snoek LB, Riksen JA, Kammenga JE. Genome-wide gene expression analysis in response to organophosphorus pesticide chlorpyrifos and diazinon in C. elegans. PLoS One. 2010; 5(8):e12145. Published 2010 Aug 16. doi:10.1371/journal.pone.0012145.
Wakatsuki S, Furuno A, Ohshima M, Araki T. Oxidative stress-dependent phosphorylation activates ZNRF1 to induce neuronal/axonal degeneration. J Cell Biol. 2015 Nov 23; 211(4):881-96. doi: 10.1083/jcb.201506102. Epub 2015 Nov 16
Weissman, B. A. & Raveh, L. Therapy against organophosphate poisoning: the importance of anticholinergic drugs with antiglutamatergic properties. Toxicol Appl Pharmacol 232, 351–358 (2008).
Winkenwerder W (2003). Environmental Exposure Report: Pesticides Final Report. Washington, DC: U.S. Department of Defense, Office of the Special Assistant to the Undersecretary of Defense (Personnel and Readiness) for Gulf War Illnesses Medical Readiness and Military Deployments.
Worek F, Aurbek N, Wille T, Eyer P, Thiermann H. Kinetic analysis of interactions of paraoxon and oximes with human, Rhesus monkey, swine, rabbit, rat and Guinea pig acetylcholinesterase. Toxicology Letters. 2011; 200:19–23
Yiu EM, Ryan MM. Genetic axonal neuropathies and neuronopathies of pre-natal and infantile onset. J Peripher Nerv Syst. 2012 Sep; 17(3):285-300. doi: 10.1111/j.1529-8027.2012.00412.x. PMID: 22971091
Zhao, C., et al., Charcot-Marie-Tooth disease type 2A caused by mutation in a microtubule motor KIF1Bbeta. Cell, 2001. 105(5): p. 587-97