
This AOP is licensed under the BY-SA license. This license allows reusers to distribute, remix, adapt, and build upon the material in any medium or format, so long as attribution is given to the creator. The license allows for commercial use. If you remix, adapt, or build upon the material, you must license the modified material under identical terms.
AOP: 436
Title
Inhibition of RALDH2 causes reduced all-trans retinoic acid levels, leading to transposition of the great arteries
Short name
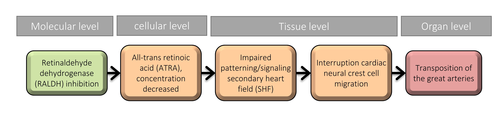
Graphical Representation
Point of Contact
Contributors
- Gina Mennen
- Arthur Author
Coaches
OECD Information Table
| OECD Project # | OECD Status | Reviewer's Reports | Journal-format Article | OECD iLibrary Published Version |
|---|---|---|---|---|
This AOP was last modified on May 26, 2024 20:39
Revision dates for related pages
| Page | Revision Date/Time |
|---|---|
| Inhibition of ALDH1A (RALDH) | November 11, 2021 14:48 |
| Decreased, all-trans retinoic acid (atRA) concentration | February 13, 2023 08:04 |
| Disruption, Progenitor cells of second heart field | February 15, 2022 10:39 |
| Neural crest cell migration, reduced | December 20, 2018 04:10 |
| transposition of the great arteries | February 15, 2022 10:47 |
| ALDH1A (RALDH), inhibition leads to Decreased, atRA concentration | November 11, 2021 15:32 |
| Decreased, atRA concentration leads to Disruption, Progenitor cells of second heart field | February 15, 2022 10:51 |
| Disruption, Progenitor cells of second heart field leads to Reduced neural crest cell migration | February 10, 2022 03:33 |
| Reduced neural crest cell migration leads to Transposition of the great arteries | February 15, 2022 10:53 |
| 4-diethylaminobenzaldehyde (DEAB) | February 15, 2022 10:55 |
| Disulfiram | August 03, 2017 10:53 |
| WIN18466 | February 15, 2022 10:56 |
| nitrofen | May 22, 2019 05:18 |
| Ethanol | April 05, 2018 06:38 |
| All-trans retionic acid | February 15, 2022 11:14 |
| Bisdiamine | May 22, 2019 05:19 |
| Vitamin A | February 15, 2022 11:15 |
| BMS-89453 | February 15, 2022 10:46 |
Abstract
The aim was to describe a linear AOP of the relationship between inhibition of retinaldehyde dehydrogenase (RALDH), an all-trans retinoic acid (ATRA) synthesizing enzyme, and the subsequent disturbance of ATRA levels that can influence impaired positioning of the great arteries as the adverse outcome (AO) during cardiovascular development. The selected molecular initiating event (MIE) is inhibition of RALDH. This MIE was selected based on robust available literature. Intermediate key events (KE) are decreased ATRA concentration, disruption of progenitor cells of the second heart field (SHF), and reduced neural crest cell (NCC) migration. Evidence for this AOP is mainly generated in chick and mouse ablation or gene mutation studies. Human evidence is limited, but comparable mechanisms between vertebrates have been reported, thereby establishing relevance due to similarities in cardiovascular development. Impaired great artery positioning is related to reduced cardiovascular function that can result in fetal/embryonic preterm deaths or require surgical intervention to correct defects in newborns. Various factors can influence the formation of the cardiovascular system and the interplay between the pharyngeal endoderm, the splanchnic mesoderm (second heart field) and the neural crest is of importance for proper development. This AOP describes the influence of the secondary heart field (SHF) on cardiac neural crest cell migration and functioning, which in turn is essential for development of the great arteries.
AOP Development Strategy
Context
Vertebrate embryo-fetal cardiovascular development involves multiple steps. The importance of all-trans retinoic acid (ATRA) in this process is well documented and has been the subject of multiple review papers (Brade et al., 2018; Duong & Waxman, 2021; Nakajima, 2019; Perl & Waxman, 2019; Stefanovic & Zaffran, 2017; S. Wang & Moise, 2019).
Cardiac progenitors
During early gastrulation at E6.5 in mice, the first cardiac progenitors are formed around the primitive streak and migrate anterior laterally to form the cardiac crescent to become the first heart field (FHF) at E7-7.5 (Stefanovic & Zaffran, 2017). An evolutionary approach to cardiac development related to the vertebrate heart was reviewed by Pérez-Pomares et al. in 2009 (Pérez-Pomares et al., 2009).
To make the cardiac crescent and primary heart tube, weak or no ATRA signaling is sufficient (Nakajima, 2019). At this stage of cardiogenesis, ATRA controls the cardiac progenitor pool size (Keegan et al., 2005; S. Wang & Moise, 2019). This early requirement of ATRA is conserved across species and restricts ventricular and atrial specification within the cardiac progenitor pool (Duong & Waxman, 2021). Before the primitive heart tube is formed, ATRA signaling is symmetrical (Nakajima, 2019).
Tube formation and anterior/posterior heart segments before looping
The heart tube is derived from the FHF at E8 in mice or after three weeks in human development (Brade et al., 2018). As the cardiac crescent folds, it will form the primitive heart tube and consequently fusion and systemic circulation can emerge (S. Wang & Moise, 2019). The FHF mainly will give rise to the left ventricle. The linear heart tube expands by cell proliferation and recruitment of additional cells that contribute to the arterial and venous poles of the heart tube and are derived from the second heart field (SHF) (Brade et al., 2018). The SHF mainly contributes to the outflow tract (OFT), the right ventricle, and part of the atria (Brade et al., 2018).
The posterior mesoderm and cardiac precursors produce ATRA, which at this stage is patterned in a caudo-rostral gradient determining the inflow-outflow poles of the heart tube (S. Wang & Moise, 2019).
Specification Second Heart Field
The SHF is specified by ISL1 (Islet-1, transcription factor and SHF specifier) positive cells and contributes to the sub-pulmonary myocardium (S. Wang & Moise, 2019).
Higher levels of ATRA promote posterior precursors of the FHF and SHF committing to the inflow tract (Hochgreb et al., 2003; Niederreither et al., 2001; Ryckebusch et al., 2008a; Sirbu et al., 2008; S. Wang & Moise, 2019). Subsequently, ATRA restricts SHF boundaries and stimulates a SHF sublineage giving rise to the outflow tract (OFT) (P. Li et al., 2010; Ma et al., 2016; Nakajima, 2019; S. Wang & Moise, 2019).
Heart tube looping / outflow tract development
As the heart tube grows, looping will occur at E9 in mice (S. Wang & Moise, 2019). During this process the straight heart tube will be remodeled by forming a coiling loop to eventually form a multichambered heart.
ATRA receptors (RARs) have been shown to be essential for cardiac looping, left-right patterning, and inflow tract development (Perl & Waxman, 2019). For proper OFT development in mice, Hox genes are necessary which are responsive to ATRA (Perl & Waxman, 2019).
Chamber formation
Chamber septation emerges at E10 in mice (S. Wang & Moise, 2019). Interaction of cardiomyocytes with epicardial, endocardial and cardiac neural crest cells (Brade et al., 2018).
ATRA is needed for the posterior heart segment to become the primitive atrium and sinus venosus (Nakajima, 2019). At later stages, ATRA stimulates growth and maturation of the ventriculi (Nakajima, 2019).
Proepicardium / Coronary vessel development
The proepicardial cells are formed between E9.5 and E11.5 in mice, migrate from a location near the sinus venosus to cover the primitive heart tube, and will form the epicardium which is the outer layer of the heart (Brade et al., 2018; S. Wang & Moise, 2019).
Mesenchymal subepicardial cells and epicardial derived cells will merge and differentiate to the coronary plexus around E11.5 in mice and subsequently coronary vessels form around the ventricle until E13.5 (Brade et al., 2018).
Several lines of evidence indicate that precision in ATRA levels and timing is important in coronary vasculature development and are reviewed by Wang and Moise (S. Wang & Moise, 2019). Coronary vasculature defects resulting from perturbed ATRA homeostasis usually concurs with myocardial expansion, vasculature development and fetal erythropoiesis (S. Wang & Moise, 2019).
myocardial expansion (ventricular wall expansion)
The FHF contributes primarily to the myocardium (S. Wang & Moise, 2019). ATRA signaling in epicardial(-derived) cells stimulates a signal promoting myocardium growth (Brade et al., 2011; S. Wang & Moise, 2019). The embryonic liver is thought to contribute to myocardial expansion through erythropoietin (EPO) secretion, which is a direct target of ATRA in the liver, and in turn induces insulin growth factor 2 (IGF2) release from the epicardium (Brade et al., 2011; S. Wang & Moise, 2019). Inactivation of EPO or its receptor resulted in ventricular hypoplasia (S. Wang & Moise, 2019; Wu et al., 1999).
Cardiac neural crest orientation and positioning
Cardiac neural crest cells (cNCCs) mainly provide patterning signals that contribute to the aortic arteries, OFT/aortopulmonary development and septation, and formation of a functional myocardium (Brade et al., 2018; Stefanovic & Zaffran, 2017; S. Wang & Moise, 2019). Additionally, cNCCs contribute to the heart valves and parasympathetic innervation (Brade et al., 2018; Stefanovic & Zaffran, 2017; S. Wang & Moise, 2019). Furthermore, preotic cNCC derived precursors contribute to vascular smooth muscle cell formation and eventually to proximal coronary arteries (Stefanovic & Zaffran, 2017). ATRA influences the cNCC migration and differentiation, which contribute to the aorticopulmonary septum / OFT (el Robrini et al., 2016; Ma et al., 2016; S. Wang & Moise, 2019).
Strategy
Summary of the AOP
Events:
Molecular Initiating Events (MIE)
Key Events (KE)
Adverse Outcomes (AO)
| Type | Event ID | Title | Short name |
|---|
| MIE | 1880 | Inhibition of ALDH1A (RALDH) | ALDH1A (RALDH), inhibition |
| KE | 1881 | Decreased, all-trans retinoic acid (atRA) concentration | Decreased, atRA concentration |
| KE | 1682 | Disruption, Progenitor cells of second heart field | Disruption, Progenitor cells of second heart field |
| KE | 1557 | Neural crest cell migration, reduced | Reduced neural crest cell migration |
| AO | 1970 | transposition of the great arteries | Transposition of the great arteries |
Relationships Between Two Key Events (Including MIEs and AOs)
| Title | Adjacency | Evidence | Quantitative Understanding |
|---|
| ALDH1A (RALDH), inhibition leads to Decreased, atRA concentration | adjacent | High | Moderate |
| Decreased, atRA concentration leads to Disruption, Progenitor cells of second heart field | adjacent | High | Low |
| Disruption, Progenitor cells of second heart field leads to Reduced neural crest cell migration | adjacent | Moderate | Low |
| Reduced neural crest cell migration leads to Transposition of the great arteries | adjacent | High | Low |
Network View
Prototypical Stressors
Life Stage Applicability
| Life stage | Evidence |
|---|---|
| Fetal | High |
Taxonomic Applicability
Sex Applicability
| Sex | Evidence |
|---|---|
| Mixed | High |
Overall Assessment of the AOP
Domain of Applicability
This AOP regarding ATRA homeostasis and cardiovascular development applies to both male and female sexes. The life stage in which the processes described as KEs and KERs are applicable is during fetal development. Strongest evidence on cardiovascular development regulation used to generate this AOP is from chicken and mouse studies with also some evidence from rat and zebrafish. Evidence exists that similar mechanisms are available in vertebrate species and therefore this AOP also applies to humans, although the evidence is not as strong.
Essentiality of the Key Events
The essentiality of each KE was determined by the impact of the upstream modified MIE or KE on the downstream KEs or AO. The level of support for essentiality of MIE and KEs within the overall AOP is high.
MIE: RALDH inhibition
The essentiality for the MIE is high because knockout and/or inhibition studies show perturbed ATRA concentrations (KE1), patterning defects in the second heart field (KE2), restricted contribution of neural crest cells (KE3), and various cardiovascular defects including transposition great arteries (AO).
Indirect evidence for essentiality of the MIE was identified as a large impact on the MIE (i.e. knockout studies) associated with an increased frequency of the downstream AO of the transposition of the great arteries. Evidence from stressors for RALDH related to cardiovascular developmental defects is also available. For example, WIN18446 (or bis-(dichloroacetyl)diamine) is an irreversible RALDH inhibitor (RALDH1, -2, and -3), that also can cause abnormal development of the aortic arch and outflow tract, coronary arteries, and the myocardium and also it can cause syndromes as tetralogy of Fallot in rats, mice and chick (Fujino et al., 2005; Kise et al., 2005; Kuribayashi & Roberts, 1993; Nishijima et al., 2000; Okamoto et al., 2004; Okishima et al., 1992; Tasaka et al., 1991; S. Wang et al., 2018).
RALDH2 is important for almost all ATRA synthesis in the heart as was shown by knockdown studies (Stefanovic & Zaffran, 2017). Mutations of the Raldh2 gene result in phenotypes characterized by prominent myocardial defects also resulting in embryonic lethality (Brade et al., 2011; el Robrini et al., 2016; Merki et al., 2005; Niederreither et al., 1999, 2001; Sorrell & Waxman, 2011; Stefanovic & Zaffran, 2017; S. Wang & Moise, 2019). Raldh2 null mice mutants that were rescued from embryo lethality showed abnormal cNCC migration (Niederreither et al., 2003). Rescued Raldh2 mouse mutant embryos also showed a disruption of the posterior limit of the SHF starting at E7.5 (Duong & Waxman, 2021; Ryckebusch et al., 2008a; Sirbu et al., 2008).
Next to RALDH, other enzymes are also involved in the formation of ATRA but also in the breakdown of ATRA.
KE1: ATRA concentration
The essentiality for the KE of disturbed ATRA levels is high as it all affects KE2, KE3 and AO.
Vertebrate embryo-fetal cardiovascular development involves multiple steps and great knowledge is available including the importance of all-trans retinoic acid (ATRA) which has been reviewed in multiple papers (Brade et al., 2018; Duong & Waxman, 2021; Nakajima, 2019; Perl & Waxman, 2019; Stefanovic & Zaffran, 2017; S. Wang & Moise, 2019). As different processes in embryodevelopment benefit from varying levels of ATRA, an ATRA gradient exists which is generated by multiple enzymes that synthesize and degrade ATRA to maintain the preferred balance (Kedishvili, 2013; Menegola et al., 2021; Tonk & Pennings, 2015). This gradient is important in SHF patterning (Nakajima, 2019).
There is also some evidence that mutants of the retinoid receptor partially revealed the mechanism of cNCC involved in cardiovascular development (Kubalak et al., 2002).
Vitamin A deficiency in embryos resulted in heart developmental defects such as septal defects, abnormalities to the inflow and outflow tract, aortic arch abnormalities and coronary malformations in quail and rat (Dersch & Zile, 1993; Heine et al., 1985; Wilson & Warkany, 1949, 1950).
KE2: SHF patterning
The essentiality is high for correct SHF patterning since different parts within the SHF are responsible for correct formation of the different anatomical positions in the developed heart as was reviewed by Nakajima in 2019 (Nakajima, 2019). Impaired development of the SHF causes cardiovascular developmental defects (Nakajima, 2019).
KE3: cNCC contribution
The contribution of cardiac neural crest cells to the development of the heart is highly essential because neural crest cell ablation studies show multiple cardiovascular developmental defects including transposed great arteries such as of the aortic arch (Plein et al., 2015).
AO: transposition great arteries
Normal cardiovascular development including normal patterning of the great arteries is essential as disruptions can lead to fetal death or teratogenic defects upon birth that hampers functioning of the newborn.
Evidence Assessment
Biological plausibility
The overall biological plausibility of the AOP was assessed as high. The role for ALDH1A2 in the synthesis of ATRA is well established as an essential component of regulating regional ATRA expression during development. The role of ATRA within cardiovascular development is highly plausible including its involvement in SHF patterning and signaling, which is important for consequent predispositioning to specific anatomical parts/occurrences in cardiovascular development.
After the initial patterning stages, the size of the cardiac progenitor pool is controlled within the anterior lateral plate mesoderm, ATRA signaling then divides the anterior and posterior SHFs (Keegan et al., 2005; S. Wang & Moise, 2019). High ATRA signaling defines the posterior boundary of the murine second heart field (Ryckebusch et al., 2008a; Sirbu et al., 2008). This is exemplified by the ATRA producing enzyme RALDH, which is expressed in posterior SHF progenitors in mice (Stefanovic et al., 2020).
The biological plausibility of the relationship between SHF signaling and cNCC contribution is moderate because the relationship between the two KEs still contain unknowns in terms of mechanistic connections. Additionally, there is an interdependent relationship between the SHF and cNCC, but also the pharyngeal endoderm plays an indispensable role in this tripartite connection (Diman et al., 2011).
There is strong biological plausibility for a link between ATRA synthesis and normal positioning of the great arteries during early development, mainly determined by mouse RALDH knouckout studies. Because of evolutionary consistencies between vertebrates (Pérez-Pomares et al., 2009), the relationship is regarded biologically plausible also in humans. No direct human evidence is available and therefore the weight of evidence is not as strong.
Empirical evidence
Dose-concordance
The quantitative understanding of dose-response relationships is limited in this AOP. 0.25-0.5 mg/ml ATRA administration specific to the anterior heart field using beads in chick embryo culture, resulted in disturbed SHF specific gene expression levels and transposition of the great arteries (Narematsu et al., 2015).
ATRA is a morphogen and the required ATRA levels are dependent on the location within the fetus for patterning and varies depending on the developmental stage (Piersma et al., 2017).
Temporal-concordance
The temporal sequence of events is strong as they are based on the biological process that are taking place. The critical period for chemical perturbations that apply to this AOP is during fetal life. The sequence in time starts with inhibition of RALDH leading to reduced ATRA synthesis. Consequently, the ATRA gradient in the SHF is disrupted resulting in an impaired pattering of the progenitors within the SHF. The progenitors within the SHF differ in signaling properties and an impaired progenitor patterning also impairs signaling to the cNCCs, which in turn fail to contribute to correct great artery development.
The relationship between the SHF and cNCC occurs at similar timepoints as they are interdependent and at the same time also communicate with the pharyngeal endoderm to be able to contribute to cardiovascular development.
Uncertainties
In mice, there is strong evidence to support the view that ATRA is important in cardiovascular development including the positioning of the great arteries. Evidence from RALDH knockout studies is also consistent. The migration and development of cNCCs not solely depends on SHF signaling. The pharyngeal endoderm also plays an important role in the maintenance and deployment of cNCCs through signaling of sonic hedgehog (Shh) (Goddeeris et al., 2007; Vincent & Buckingham, 2010). In the absence of Shh, the development of proper pharyngeal arches and OFT is affected (Vincent & Buckingham, 2010). Additionally, a possible feedback loop exists between SHF signaling to cNCCs, since ablation of cNCCs results in SHF over proliferation because of excessive Fgf8 signaling (Rochais et al., 2009). Furthermore, NCC deletion of Smad4 leads to abnormal SHF patterning and a shorter OFT. Lastly, Tbx3 loss in NCCs and pharyngeal endoderm also resulted in SHF over proliferation and a shorter OFT (Rochais et al., 2009).
Known Modulating Factors
Quantitative Understanding
This AOP is of qualitative understanding. Quantitative data between chemical potency and perturbations are insufficient. This relates to the mainly strong evidence of the MIE coming from gene knockout studies. Furthermore, ATRA is a morphogen and the required ATRA levels are dependent on the location within the fetus for patterning and varies depending on the developmental stage (Piersma et al., 2017).
Considerations for Potential Applications of the AOP (optional)
References
Brade, T., Kumar, S., Cunningham, T. J., Chatzi, C., Zhao, X., Cavallero, S., Li, P., Sucov, H. M., Ruiz-Lozano, P., & Duester, G. (2011). Retinoic acid stimulates myocardial expansion by induction of hepatic erythropoietin which activates epicardial Igf2. Development, 138(1), 139–148. https://doi.org/10.1242/dev.054239
Brade, T., Pane, L. S., Moretti, A., Chien, K. R., & Laugwitz, K.-L. (2018). Embryonic Heart Progenitors and Cardiogenesis. 1–18. https://doi.org/10.1101/cshperspect.a013847
Dersch, H., & Zile, M. H. (1993). Induction of normal cardiovascular development in the vitamin A-deprived quail embryo by natural retinoids. Developmental Biology, 160(2), 424–433. https://doi.org/10.1006/dbio.1993.1318
Diman, N. Y. S. G., Remacle, S., Bertrand, N., Picard, J. J., Zaffran, S., & Rezsohazy, R. (2011). A retinoic acid responsive Hoxa3 transgene expressed in embryonic pharyngeal endoderm, cardiac neural crest and a subdomain of the second heart field. PloS One, 6(11). https://doi.org/10.1371/JOURNAL.PONE.0027624
Duong, T. B., & Waxman, J. S. (2021). Patterning of vertebrate cardiac progenitor fields by retinoic acid signaling. Genesis (New York, N.Y. : 2000), e23458. https://doi.org/10.1002/dvg.23458
el Robrini, N., Etchevers, H. C., Ryckebüsch, L., Faure, E., Eudes, N., Niederreither, K., Zaffran, S., & Bertrand, N. (2016a). Cardiac outflow morphogenesis depends on effects of retinoic acid signaling on multiple cell lineages. Developmental Dynamics, 245(3), 388–401. https://doi.org/10.1002/dvdy.24357
el Robrini, N., Etchevers, H. C., Ryckebüsch, L., Faure, E., Eudes, N., Niederreither, K., Zaffran, S., & Bertrand, N. (2016b). Cardiac outflow morphogenesis depends on effects of retinoic acid signaling on multiple cell lineages. Developmental Dynamics, 245(3), 388–401. https://doi.org/10.1002/dvdy.24357
Fujino, H., Nakagawa, M., Nishijima, S., Okamoto, N., Hanato, T., Watanabe, N., Shirai, T., Kamiya, H., & Takeuchi, Y. (2005). Morphological differences in cardiovascular anomalies induced by bis-diamine between Sprague-Dawley and Wistar rats. Congenital Anomalies, 45(2), 52–58. https://doi.org/10.1111/j.1741-4520.2005.00063.x
Goddeeris, M. M., Schwartz, R., Klingensmith, J., & Meyers, E. N. (2007). Independent requirements for Hedgehog signaling by both the anterior heart field and neural crest cells for outflow tract development. Development (Cambridge, England), 134(8), 1593–1604. https://doi.org/10.1242/DEV.02824
Heine, U. I., Roberts, A. B., Munoz, E. F., Roche, N. S., & Sporn, M. B. (1985). Effects of retinoid deficiency on the development of the heart and vascular system of the quail embryo. Virchows Archiv. B, Cell Pathology Including Molecular Pathology, 50(2), 135–152. https://doi.org/10.1007/BF02889897
Hochgreb, T., Linhares, V. L., Menezes, D. C., Sampaio, A. C., Yan, C. Y. I., Cardoso, W. v., Rosenthal, N., & Xavier-Neto, J. (2003). A caudorostral wave of RALDH2 conveys anteroposterior information to the cardiac field. Development, 130(22), 5363–5374. https://doi.org/10.1242/DEV.00750
Kedishvili, N. Y. (2013). Enzymology of retinoic acid biosynthesis and degradation. Journal of Lipid Research, 54(7), 1744–1760. https://doi.org/10.1194/JLR.R037028
Keegan, B. R., Feldman, J. L., Begemann, G., Ingham, P. W., & Yelon, D. (2005). Retinoic acid signaling restricts the cardiac progenitor pool. Science (New York, N.Y.), 307(5707), 247–249. https://doi.org/10.1126/SCIENCE.1101573
Kise, K., Nakagawa, M., Okamoto, N., Hanato, T., Watanabe, N., Nishijima, S., Fujino, H., Takeuchi, Y., & Shiraishi, I. (2005). Teratogenic effects of bis-diamine on the developing cardiac conduction system. Birth Defects Research Part A - Clinical and Molecular Teratology, 73(8), 547–554. https://doi.org/10.1002/bdra.20163
Kubalak, S. W., Hutson, D. R., Scott, K. K., & Shannon, R. A. (2002). Elevated transforming growth factor β2 enhances apoptosis and contributes to abnormal outflow tract and aortic sac development in retinoic X receptor α knockout embryos. Development, 129(3), 733–746. https://doi.org/10.1242/dev.129.3.733
Kuribayashi, T., & Roberts, W. C. (1993). Tetralogy of fallot, truncus arteriosus, abnormal myocardial architecture and anomalies of the aortic arch system induced by bis-diamine in rat fetuses. Journal of the American College of Cardiology, 21(3), 768–776. https://doi.org/10.1016/0735-1097(93)90111-D
Li, P., Pashmforoush, M., & Sucov, H. M. (2010). Retinoic Acid Regulates Differentiation of the Secondary Heart Field and TGFβ-Mediated Outflow Tract Septation. Developmental Cell, 18(3), 480–485. https://doi.org/10.1016/J.DEVCEL.2009.12.019/ATTACHMENT/B413E05D-04E2-4F76-9417-72BF1FD02515/MMC1.PDF
Ma, M., Li, P., Shen, H., Estrada, K. D., Xu, J., Kumar, S. R., & Sucov, H. M. (2016). Dysregulated endocardial TGFβ signaling and mesenchymal transformation result in heart outflow tract septation failure. Developmental Biology, 409(1), 272–276. https://doi.org/10.1016/J.YDBIO.2015.09.021
Menegola, E., Veltman, C. H. J., Battistoni, M., di Renzo, F., Moretto, A., Metruccio, F., Beronius, A., Zilliacus, J., Kyriakopoulou, K., Spyropoulou, A., Machera, K., van der Ven, L. T. M., & Luijten, M. (2021). An adverse outcome pathway on the disruption of retinoic acid metabolism leading to developmental craniofacial defects. Toxicology, 458. https://doi.org/10.1016/J.TOX.2021.152843
Merki, E., Zamora, M., Raya, A., Kawakami, Y., Wang, J., Zhang, X., Burch, J., Kubalak, S. W., Kaliman, P., Belmonte, J. C. I., Chien, K. R., & Ruiz-Lozano, P. (2005). Epicardial retinoid X receptor alpha is required for myocardial growth and coronary artery formation. Proceedings of the National Academy of Sciences of the United States of America, 102(51), 18455–18460. https://doi.org/10.1073/PNAS.0504343102
Nakajima, Y. (2019). Retinoic acid signaling in heart development. Genesis, 57(7). https://doi.org/10.1002/dvg.23300
Narematsu, M., Kamimura, T., Yamagishi, T., Fukui, M., & Nakajima, Y. (2015). Impaired development of left anterior heart field by ectopic retinoic acid causes transposition of the great arteries. Journal of the American Heart Association, 4(5). https://doi.org/10.1161/JAHA.115.001889
Niederreither, K., Subbarayan, V., Dolle, P., & Chambon, P. (1999). Embryonic retinoic acid synthesis is essential for early mouse post-implantation development. Nature Genetics, 21(4), 444–448. https://doi.org/10.1038/7788
Niederreither, K., Vermot, J., le Roux, I., Schuhbaur, B., Chambon, P., & Dollé, P. (2003). The regional pattern of retinoic acid synthesis by RALDH2 is essential for the development of posterior pharyngeal arches and the enteric nervous system. Development, 130(11), 2525–2534. https://doi.org/10.1242/dev.00463
Niederreither, K., Vermot, J., Messaddeq, N., Schuhbaur, B., Chambon, P., & Dollé, P. (2001). Embryonic retinoic acid synthesis is essential for heart morphogenesis in the mouse. Development (Cambridge, England), 128(7), 1019–1031. https://doi.org/10.1242/dev.128.7.1019
Nishijima, S., Nakagawa, M., Fujino, H., Hanato, T., Okamoto, N., & Shimada, M. (2000). Teratogenic effects of bis-diamine on early embryonic rat heart: An in vitro study. Teratology, 62(2), 115–122. https://doi.org/10.1002/1096-9926(200008)62:2<115::aid-tera8>3.0.co;2-%23
Okamoto, N., Nakagawa, M., Fujino, H., Nishijima, S., Hanato, T., Narita, T., Takeuchi, Y., & Imanaka-Yoshida, K. (2004). Teratogenic Effects of Bis-diamine on the Developing Myocardium. Birth Defects Research Part A - Clinical and Molecular Teratology, 70(3), 132–141. https://doi.org/10.1002/bdra.20001
Okishima, T., Takamura, K., Matsuoka, Y., Ohdo, S., & Hayakawa, K. (1992). Cardiovascular anomalies in chick embryos produced by bis‐diamine in dimethylsulfoxide. Teratology, 45(2), 155–162. https://doi.org/10.1002/tera.1420450209
Pérez-Pomares, J. M., González-Rosa, J. M., & Muñoz-Chápuli, R. (2009). Building the vertebrate heart - An evolutionary approach to cardiac development. International Journal of Developmental Biology, 53(8–10), 1427–1443. https://doi.org/10.1387/IJDB.072409JP
Perl, E., & Waxman, J. S. (2019). Reiterative Mechanisms of Retinoic Acid Signaling during Vertebrate Heart Development. Journal of Developmental Biology, 7(2). https://doi.org/10.3390/jdb7020011
Piersma, A. H., Hessel, E. v., & Staal, Y. C. (2017). Retinoic acid in developmental toxicology: Teratogen, morphogen and biomarker. Reproductive Toxicology, 72, 53–61. https://doi.org/10.1016/J.REPROTOX.2017.05.014
Plein, A., Fantin, A., & Ruhrberg, C. (2015). Neural crest cells in cardiovascular development. In Current Topics in Developmental Biology (1st ed., Vol. 111). Elsevier Inc. https://doi.org/10.1016/bs.ctdb.2014.11.006
Rochais, F., Mesbah, K., & Kelly, R. G. (2009). Signaling pathways controlling second heart field development. Circulation Research, 104(8), 933–942. https://doi.org/10.1161/CIRCRESAHA.109.194464
Ryckebusch, L., Wang, Z., Bertrand, N., Lin, S. C., Chi, X., Schwartz, R., Zaffran, S., & Niederreither, K. (2008). Retinoic acid deficiency alters second heart field formation. Proceedings of the National Academy of Sciences of the United States of America, 105(8), 2913–2918. https://doi.org/10.1073/PNAS.0712344105
Sirbu, I. O., Zhao, X., & Duester, G. (2008). Retinoic acid controls heart anteroposterior patterning by down-regulating Isl1 through the Fgf8 pathway. Developmental Dynamics : An Official Publication of the American Association of Anatomists, 237(6), 1627–1635. https://doi.org/10.1002/DVDY.21570
Sorrell, M. R. J., & Waxman, J. S. (2011). Restraint of Fgf8 signaling by retinoic acid signaling is required for proper heart and forelimb formation. Developmental Biology, 358(1), 44–55. https://doi.org/10.1016/J.YDBIO.2011.07.022
Stefanovic, S., Laforest, B., Desvignes, J. P., Lescroart, F., Argiro, L., Maurel-Zaffran, C., Salgado, D., Plaindoux, E., de Bono, C., Pazur, K., Théveniau-Ruissy, M., Béroud, C., Puceat, M., Gavalas, A., Kelly, R. G., & Zaffran, S. (2020). Hox-dependent coordination of mouse cardiac progenitor cell patterning and differentiation. ELife, 9, 1–32. https://doi.org/10.7554/ELIFE.55124
Stefanovic, S., & Zaffran, S. (2017a). Mechanisms of retinoic acid signaling during cardiogenesis. Mechanisms of Development, 143, 9–19. https://doi.org/10.1016/j.mod.2016.12.002
Stefanovic, S., & Zaffran, S. (2017b). Mechanisms of retinoic acid signaling during cardiogenesis. Mechanisms of Development, 143, 9–19. https://doi.org/10.1016/j.mod.2016.12.002
Tasaka, H., Takenaka, H., Okamoto, N., Onitsuka, T., Koga, Y., & Hamada, M. (1991). Abnormal development of cardiovascular systems in rat embryos treated with bisdiamine. Teratology, 43(3), 191–200. https://doi.org/10.1002/tera.1420430303
Tonk, E. C. M., & Pennings, J. L. A. (2015). An adverse outcome pathway framework for neural tube and axial defects mediated by modulation of retinoic acid homeostasis. Reproductive Toxicology, 55, 104–113. https://doi.org/10.1016/J.REPROTOX.2014.10.008
Vincent, S. D., & Buckingham, M. E. (2010). How to make a heart. The origin and regulation of cardiac progenitor cells. Current Topics in Developmental Biology, 90(C), 1–41. https://doi.org/10.1016/S0070-2153(10)90001-X
Wang, S., Huang, W., Castillo, H. A., Kane, M. A., Xavier-Neto, J., Trainor, P. A., & Moise, A. R. (2018). Alterations in retinoic acid signaling affect the development of the mouse coronary vasculature. Developmental Dynamics, 247(8), 976–991. https://doi.org/10.1002/dvdy.24639
Wang, S., & Moise, A. R. (2019). Recent insights on the role and regulation of retinoic acid signaling during epicardial development. Genesis, 57(7). https://doi.org/10.1002/dvg.23303
WILSON, J. G., & WARKANY, J. (1949). Aortic-arch and cardiac anomalies in the offspring of vitamin A deficient rats. The American Journal of Anatomy, 85(1), 113–155. https://doi.org/10.1002/AJA.1000850106
WILSON, J. G., & WARKANY, J. (1950). Cardiac and aortic arch anomalies in the offspring of vitamin A deficient rats correlated with similar human anomalies. Pediatrics, 5(4), 708–725. https://doi.org/10.1542/peds.5.4.708
Wu, H., Lee, S. H., Gao, J., Liu, X., & Iruela-Arispe, M. L. (1999). Inactivation of erythropoietin leads to defects in cardiac morphogenesis. Development, 126(16), 3597–3605. https://doi.org/10.1242/DEV.126.16.3597